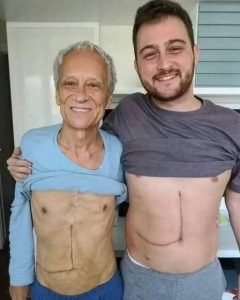
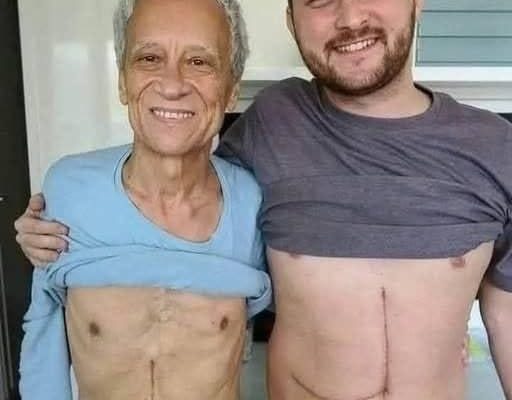
A young man’s decision to save his father’s life through a liver donation is often described as one of the most selfless acts a person can make. It is a story that circulates widely online: a son stepping forward without hesitation, offering part of his own body so that his father might live. But sometimes, in the more sensationalized versions of these stories, the narrative takes a darker turn—ending in unexpected complications, emotional devastation, or tragic outcomes that leave families shattered.
What follows is a carefully written, fictionalized composite story based on common themes found in medical transplant experiences. It is not a report of any specific real event, but rather a narrative exploration of what can happen when love, medicine, and human vulnerability collide in complex ways.
The story begins in a small suburban town, where a 52-year-old father is diagnosed with advanced liver disease. Years of silent progression—fatty liver complications, undiagnosed hepatitis, and the cumulative toll of lifestyle factors—finally culminate in a diagnosis that changes everything: without a transplant, he may not survive more than a few months.
His son, a 24-year-old college graduate, is immediately tested as a potential donor. In most countries, living liver donation is possible because the liver is one of the few organs capable of regenerating. Doctors explain the risks carefully: this is not a minor procedure. It involves removing a significant portion of a healthy person’s liver, performing major abdominal surgery, and accepting the possibility—however rare—of serious complications.
But the son does not hesitate.
“I’ll do it,” he says before the medical team even finishes their explanation.
To him, it is not a decision. It is instinct.
Pre-surgical evaluations take weeks. Blood tests, imaging scans, psychological assessments. The medical team wants to ensure that the donor is fully informed and emotionally stable. They also want to confirm compatibility. The son passes every test. He is young, healthy, and physically strong. Doctors call him an “excellent candidate.”
In the hospital, the father and son share a quiet room the night before surgery. There are few words. The father tries to refuse the donation one last time, overwhelmed by guilt.
But the son simply says, “You raised me. This is what I can do for you.”
Neither of them sleeps much that night.
The surgery is scheduled for early morning. Two operating rooms are prepared side by side—one for the donor, one for the recipient. A coordinated team of surgeons begins the complex procedure.
For the father, the diseased liver is carefully removed. For the son, surgeons extract a portion—often the right lobe in adult-to-adult donations—meticulously preserving blood vessels and bile ducts.
In most cases, both surgeries go as planned. Complication rates in modern transplant medicine are low, but never zero.
And in this story, something begins to go wrong.
During the son’s recovery in the intensive care unit, he initially appears stable. Vital signs are monitored continuously. Nurses note that he is groggy but responsive. His family is told that the surgery was successful.
But within hours, subtle warning signs emerge.
His blood pressure drops unexpectedly. His abdominal pain intensifies beyond what is typical for post-operative recovery. The medical team orders urgent imaging. What they discover is rare but serious: internal bleeding near the resection site of the liver.
A second emergency procedure is required.
In the operating room once again, surgeons work quickly to locate and control the source of the bleeding. The human liver, while regenerative, is also highly vascular, meaning even small complications can escalate rapidly. Sutures are reinforced, damaged vessels are repaired, and blood transfusions are administered.
For a time, the situation stabilizes.
But complications continue in a cascade effect that sometimes occurs in major surgery: infection risk rises, liver function fluctuates, and the body struggles to adapt to the sudden loss of tissue.
Meanwhile, the father’s transplant initially appears successful. His body begins accepting the new liver segment. There is cautious optimism in the transplant unit.
Two lives, once deeply connected, are now tied together in two different ICUs—each fighting their own battle.
Over the next several days, the son’s condition worsens. Despite aggressive treatment, he develops a severe post-surgical infection. Antibiotics are administered, and additional procedures are performed to drain fluid buildup in the abdominal cavity.
His family gathers at his bedside. The same hospital that once felt like a place of hope now feels like a place of suspended grief.
Doctors are careful in their language. They emphasize uncertainty. They explain that while such outcomes are rare, they can occur even in highly advanced medical systems.
The family struggles to reconcile the contradiction: a surgery meant to save a life has placed another life in danger.
Eventually, after a prolonged and difficult hospitalization, the son’s condition reaches a critical point. His organs begin to fail under the strain of complications. Despite every intervention, the medical team is unable to reverse the trajectory.
He passes away surrounded by his family.
The father, recovering in the adjacent unit, is not told immediately. Medical staff and relatives struggle with how to deliver the news while he is still medically fragile. When he finally learns what has happened, his recovery becomes emotionally complicated in ways medicine cannot easily measure.
He survives—but with a grief that becomes inseparable from his survival.
In the weeks that follow, the family is left with a painful duality. The father is alive because of his son’s sacrifice. Yet that very sacrifice has become the source of unimaginable loss.
Doctors later describe the case in more clinical terms: a rare but known set of complications following living donor liver transplantation. Medical journals often emphasize that living liver donation is generally safe, with high survival rates for both donor and recipient. But behind those statistics are individual stories—some triumphant, others tragic.
Ethicists often point to cases like this to highlight the emotional complexity of living organ donation. Unlike deceased donation, living donation carries an inherent paradox: one person undergoes major surgery not for their own health, but for the survival of another.
The psychological weight of that decision is immense. Families must navigate hope, fear, obligation, and love—all at once.
In most cases, outcomes are positive. Many donors go on to live completely normal lives after recovery. But medicine, by its nature, cannot eliminate risk entirely.
In the end, this fictionalized narrative serves as a reminder of both the power and fragility of modern transplant medicine. A liver donation can mean the difference between life and death. It can also carry risks that no amount of preparation can fully erase.
The son in this story is remembered not for the outcome, but for the intention behind his choice. A decision made out of love, without hesitation, in the hope of saving a parent’s life.
And the father, continuing to live, carries forward a legacy that is both life-giving and heartbreaking—an everyday reminder that survival sometimes comes at a cost that words can barely contain.